This month we saw a cute little patient, an axolotl (Mexican salamander) named Axolotl! To see pictures of other axolotls and learn more about them, see this Wikipedia entry: https://en.wikipedia.org/wiki/Axolot
Unlike other amphibians, the axolotl starts out like a tadpole, and never trade their gills for lungs; instead they live their entire lives in the water.
Axolotls have a bad habit of eating small rocks and other material in their enclosure. In fact, this is the number one health problem of axolotls in general (in both pet and laboratory settings), as they have very few illnesses if they are fed and cared for correctly. For this reason, it’s recommended to house them in a plain aquarium, or with objects too big to get into their mouths.
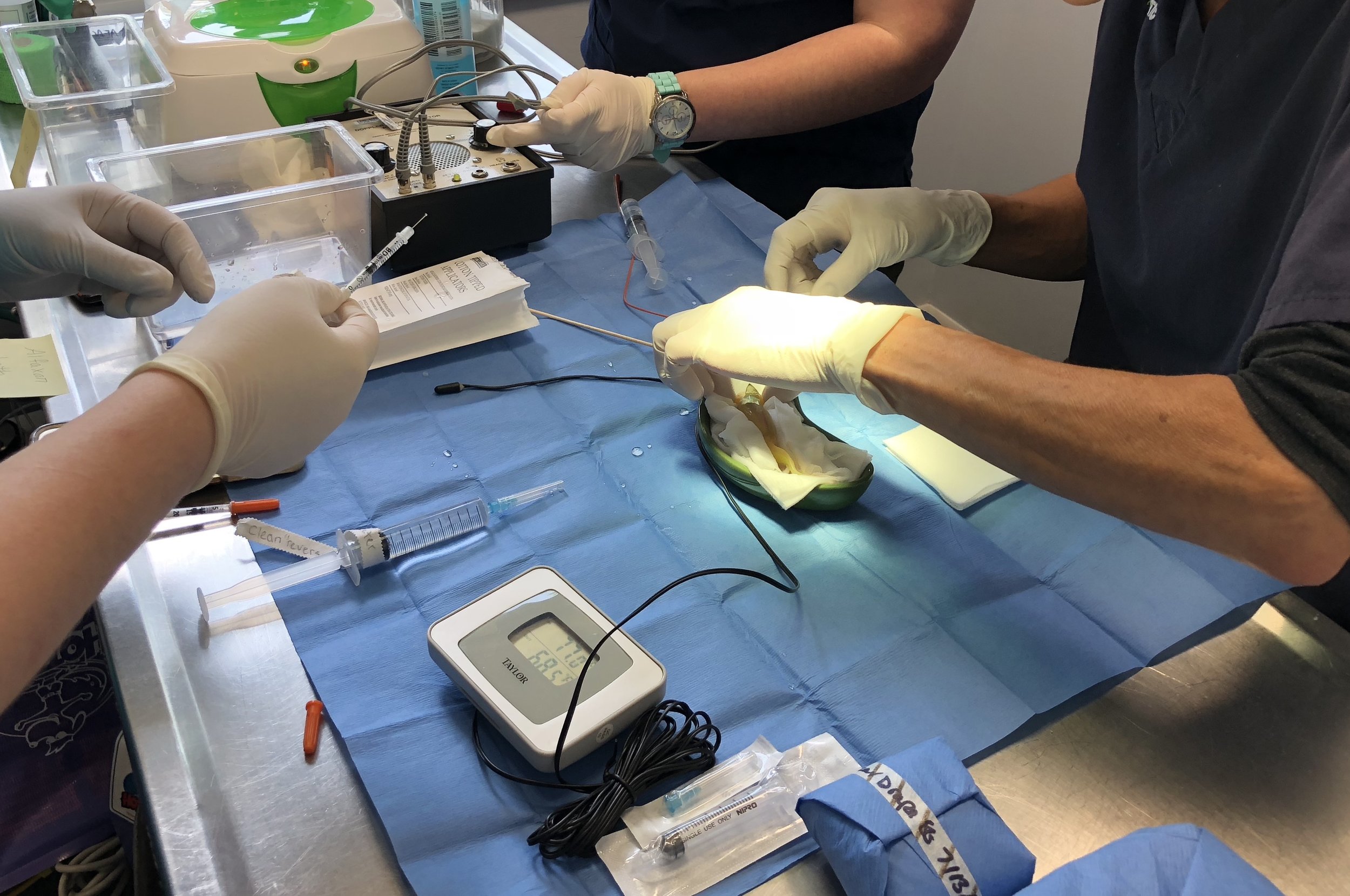
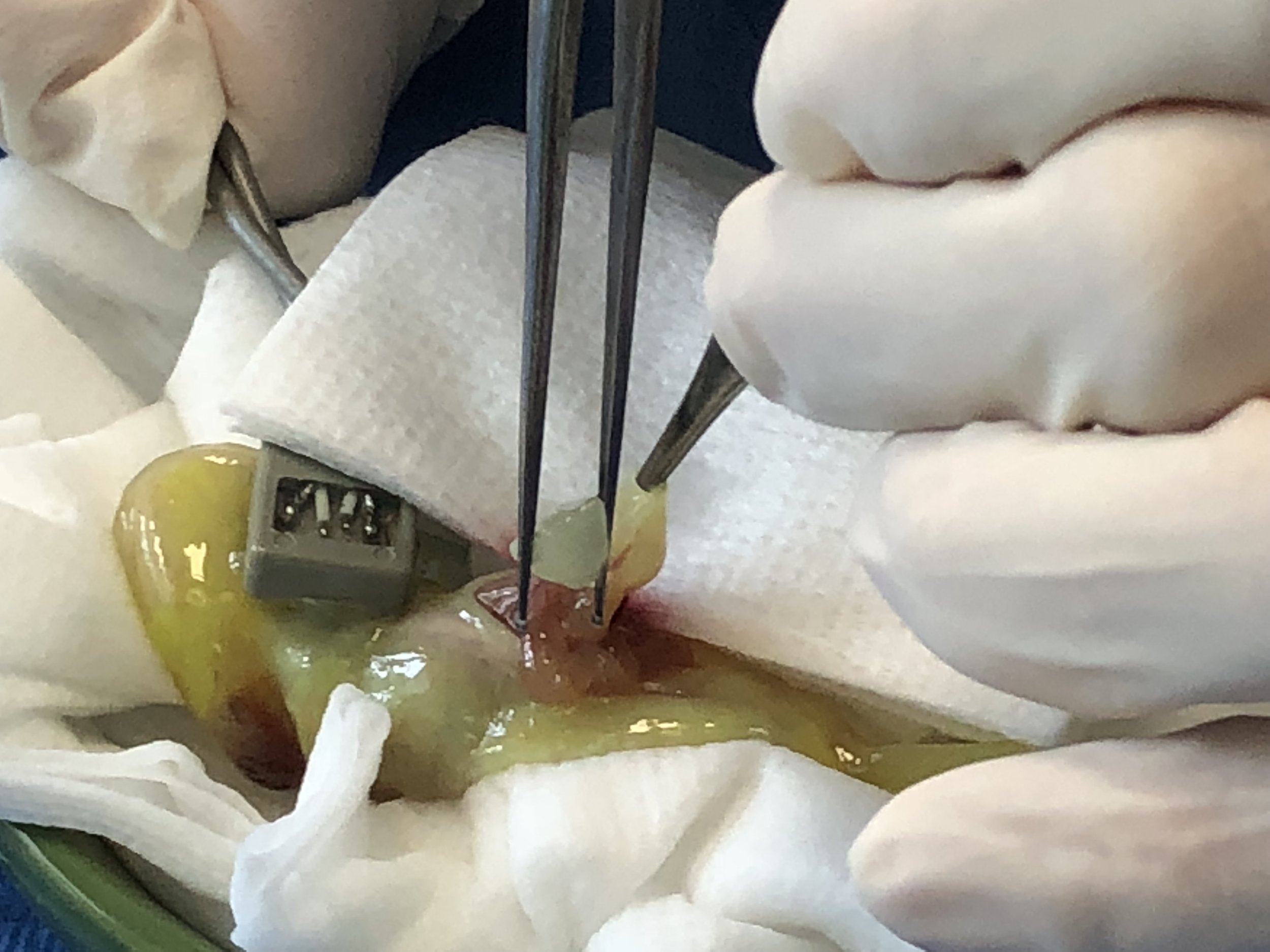
This axolotl decided to eat a fairly large number of rocks of all sizes. His owner quickly removed the gravel, and he proceeding to “eliminate” most of them…except for 6 really large rocks far too big to come out that way. They were also too big and irregular to simply pull out of his stomach with an endoscope.
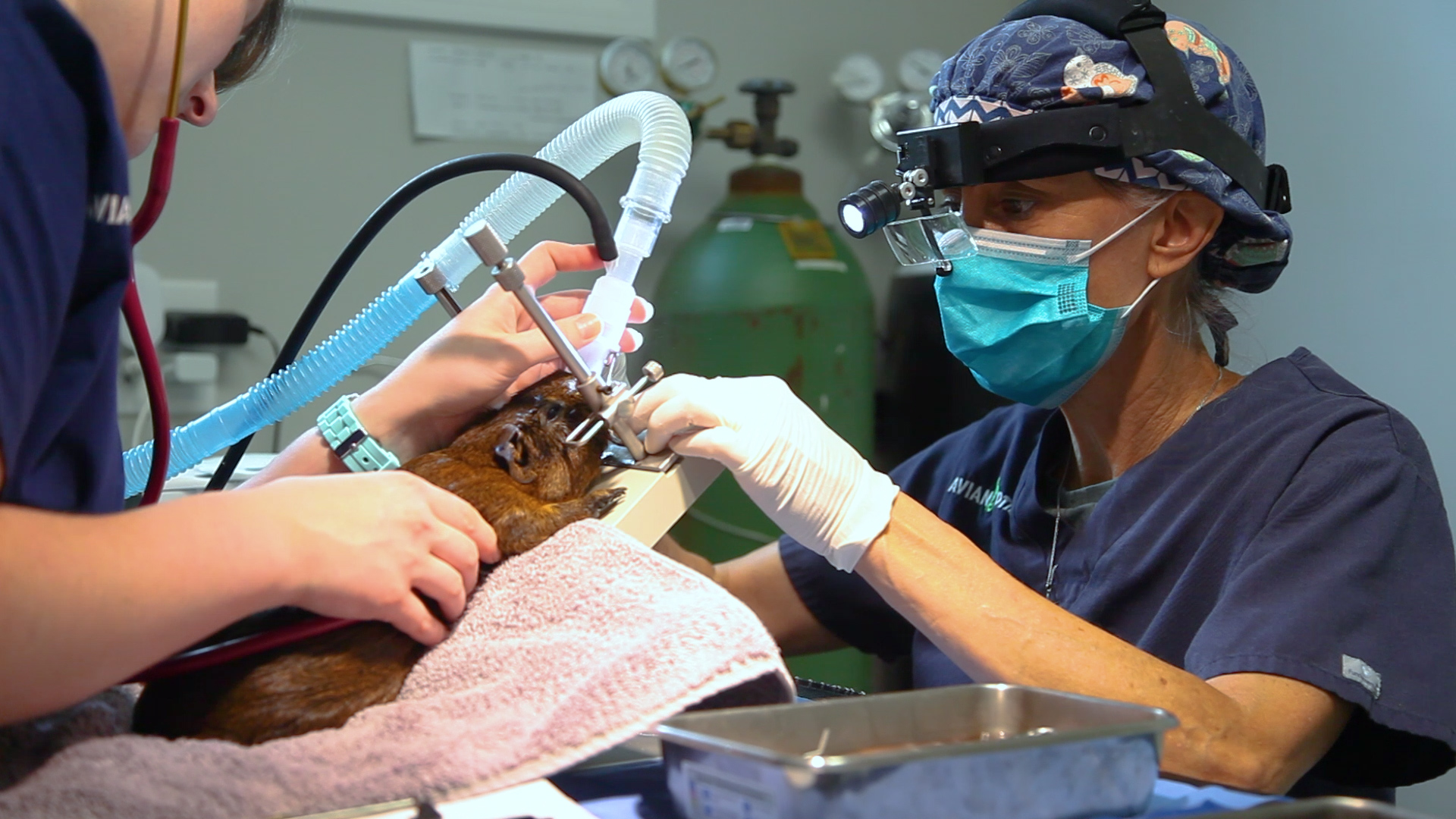
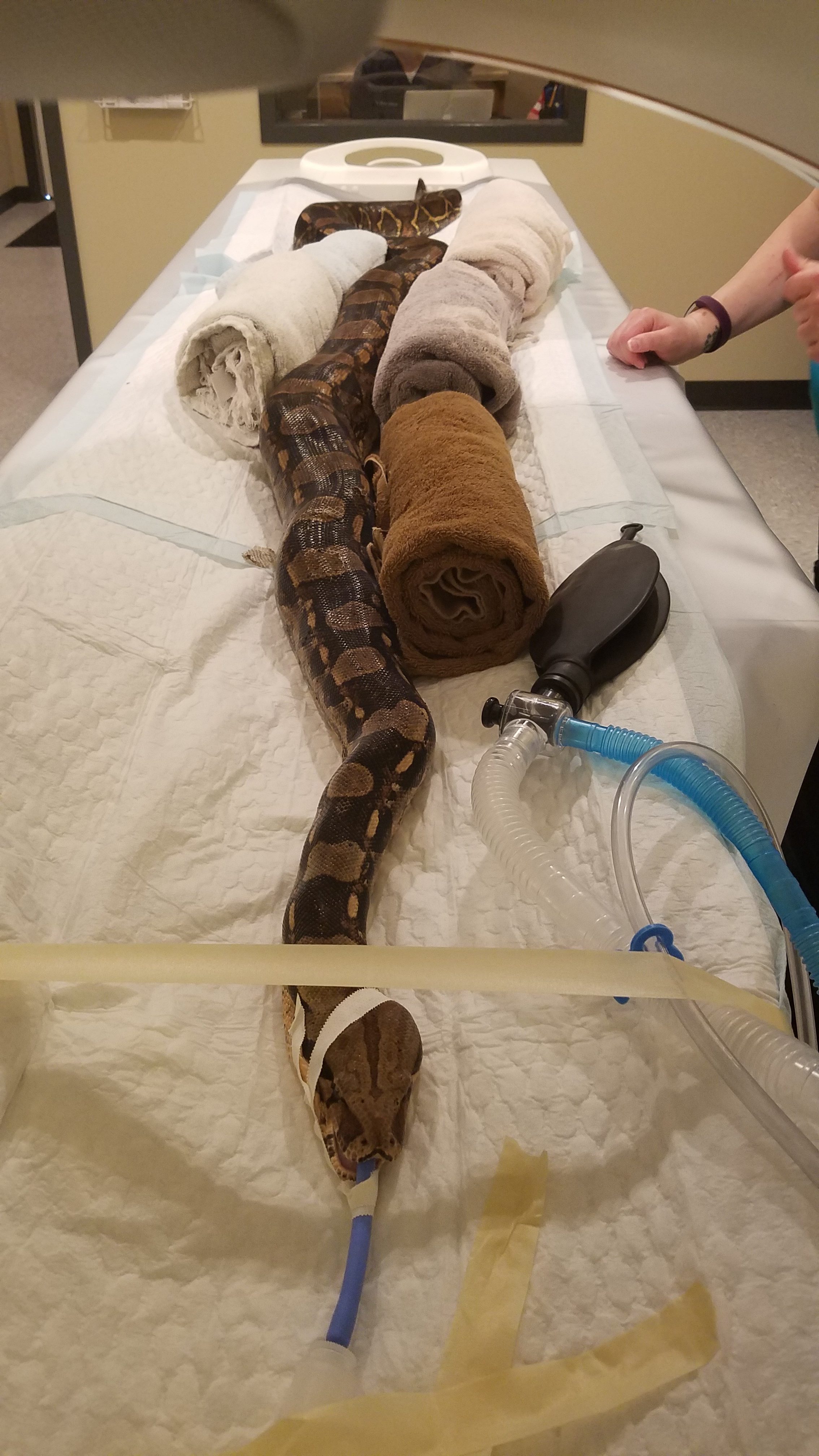
So how does one anesthetize an aquatic axolotl?
Some interesting current publications show that the best way to keep them asleep for surgery is to bathe their skin and gills with an anesthetic water bath.
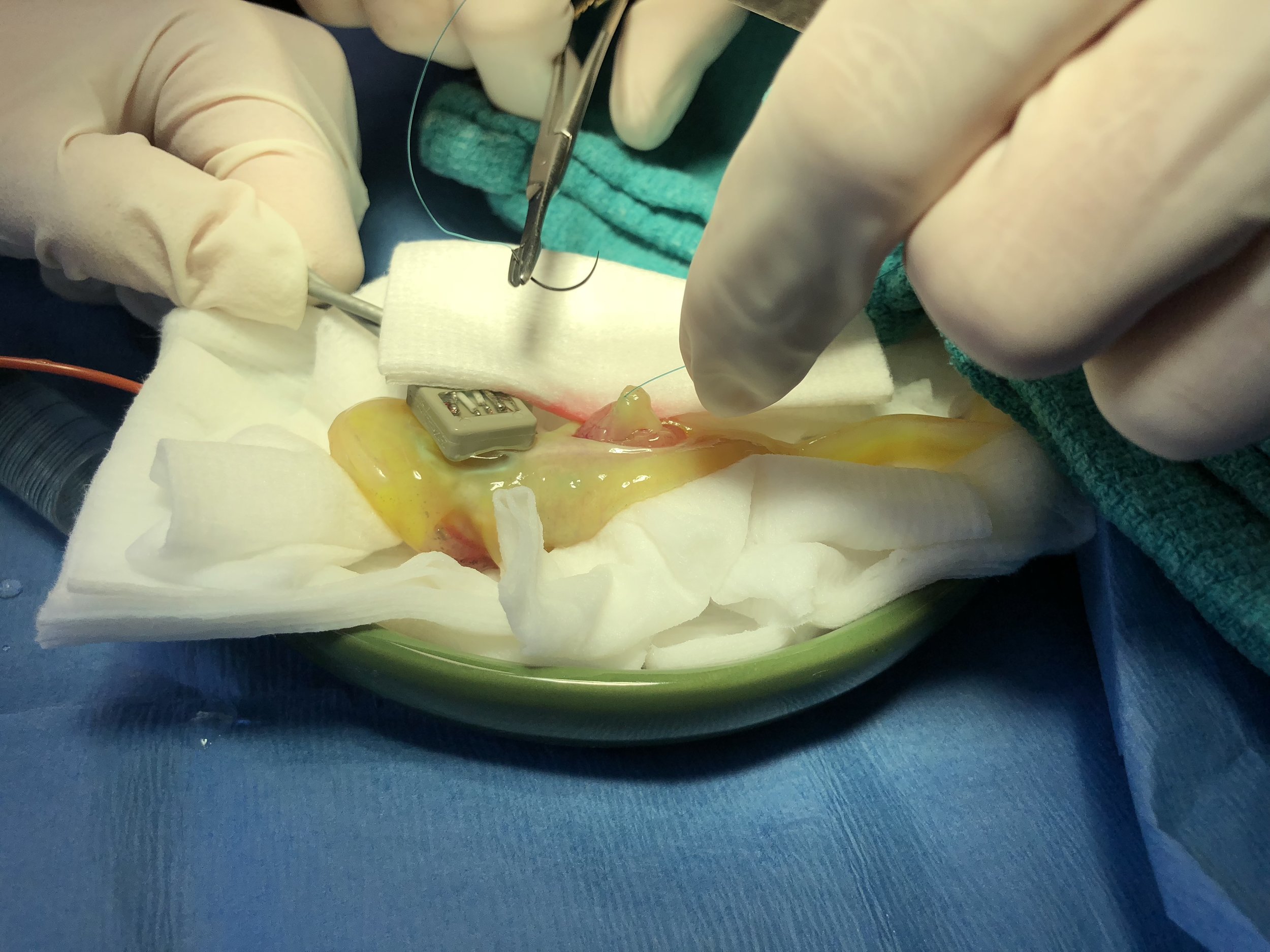
Hopefully the sutures will stay secure, and he will make a full recovery-and NO more rocks!
The axolotl was sent home the next day, and we hear he is already eating small meals.




































 This little Chinese Water Dragon went for a car ride to come see us recently. Since it’s safest for him and all other pets to travel in secure carriers and we require all pets to be contained in the waiting room, he came to the clinic in the best carrier his owners had on hand. To make him comfortable, his owners put in a nice fleece blanket and something to hide in. However, when he arrived at the clinic and his carrier was opened, he was missing! We quickly called his owners. They carefully checked their car and found him hiding out. Luckily, there was no harm done and he did well for his visit. Next time, we’re sure he will come in a carrier with much smaller bars!
Are you unsure about what kind of carrier your exotic pet needs? We have seen just about EVERYTHING, so we can always let you know what works best! Give us a call and we would be happy to give you some recommendations!
This little Chinese Water Dragon went for a car ride to come see us recently. Since it’s safest for him and all other pets to travel in secure carriers and we require all pets to be contained in the waiting room, he came to the clinic in the best carrier his owners had on hand. To make him comfortable, his owners put in a nice fleece blanket and something to hide in. However, when he arrived at the clinic and his carrier was opened, he was missing! We quickly called his owners. They carefully checked their car and found him hiding out. Luckily, there was no harm done and he did well for his visit. Next time, we’re sure he will come in a carrier with much smaller bars!
Are you unsure about what kind of carrier your exotic pet needs? We have seen just about EVERYTHING, so we can always let you know what works best! Give us a call and we would be happy to give you some recommendations!


















